There is an inherent tension in the field of public health: How do you effect the greatest good for the greatest number of people without denying them personal freedom? It might seem reasonable to impose a quarantine during an outbreak of a highly infectious disease with a terrifying fatality rate, but how should we regulate factors that contribute to slow killers such as diabetes, hypertension, and obesity?
Since 1980, the rate of obesity has been increasing so steadily that nearly half of all Americans are expected to be obese by 2020. As our waistlines grow, public health officials are looking for ways to shrink our appetites. According to obesity research, the average American’s weight is not the only thing increasing. The number of restaurants in the United States is at a record high. People eat restaurant food more often than ever before, and people who report high consumption of restaurant food—particularly fast food—are heavier than those who eat food cooked at home.
But does eating in restaurants cause obesity? David Matsa (Assistant Professor of Finance at the Kellogg School of Management) and Michael Anderson (Assistant Professor of Agricultural and Resource Economics at the University of California, Berkeley) conducted a comprehensive study of the question. “There are arguments that could lead you to believe there would be a causal relationship, so we wanted to understand if this was true,” Matsa says.
Many policy makers assume that eating out does contribute to obesity. Los Angeles will not permit new fast-food restaurants to open in South L.A., an area beset by obesity and poverty. Following in New York State’s footsteps, California and the cities of Philadelphia, Portland, and Seattle are moving to require chain restaurants to print nutrition information, including calorie counts, on menus. Washington State is considering a tax on fat-laden foods such as burgers and fries.
Matsa and Anderson addressed the problem by analyzing real-world data, including surveys on calorie consumption and maps of restaurant availability and accessibility. Matsa notes that theirs is the only study of restaurant proximity and obesity separates supply from demand in addressing a fundamental question: Does the number of nearby restaurants cause people to eat more, or are restaurants more numerous because people are eating more?
Roadside Diners
Matsa and Anderson wanted to know if people who live closer to restaurants weigh more than those who live farther away. A meal’s tab is not the only cost of eating out: The farther a consumer lives from a restaurant, the higher the cost in fuel, time, and effort. If cost was a deciding factor, those who lived closer to dining establishments would be more likely to eat out and—if restaurants were indeed at fault—would be more likely to be obese.
Matsa and Anderson looked at data from the Behavioral Risk Factors Surveillance System. Each year, state health departments phone a sample of residents and ask them about their habits and health, including their height and weight. These measures are used to calculate respondents’ body mass indexes, an estimate of body fat. A body mass index of 25 or higher indicates that a person is overweight; 30 or higher is considered obese.
Eleven states provided data that included the first six digits of the respondents’ phone numbers. Because landline numbers are tied to geographic locations, Matsa and Anderson could determine respondents’ proximity to highways. In the rural United States, restaurants typically are clustered around limited-access highway exits.
Matsa and Anderson focused on rural areas—those at least 30 miles from urban areas with fewer than 80 people per square mile—because nearly everyone in more densely populated urban settings has easy access to restaurants. The highway model also ensures that the abundance of nearby restaurants is not a factor of their use by local residents. Because restaurants are often located near highways to serve customers passing through, their density in those areas is higher than what the local population would support on its own. Had they not used the highway approach, Matsa and Anderson might have inadvertently sampled a population with a fondness for restaurant food that increased both their waistlines and the number of local restaurants.
“There is a lot of work relating body mass to how often people eat out, to the growth in restaurant density, and even to how far restaurants are located from schools. But none of those studies tries to account for consumer preferences or examines variation in the supply of restaurants, which is what we were trying to accomplish with the highway method,” Matsa says.
Using highways as a guide revealed some surprising results. Matsa and Anderson found that respondents’ proximity to a highway, and therefore to restaurants, did not lead to increased body mass. No matter how near to or far from a highway respondents lived, body masses were nearly the same (see Figure 1).
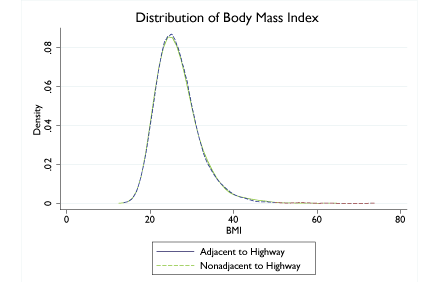
Figure 1: Distribution of Body Mass Index in Towns Adjacent and Nonadjacent to Interstate Highways
Still, Matsa and Anderson needed a finer level of detail to eliminate the possibility that all the respondents were eating at restaurants—or not—regardless of how far they lived from a highway, so they surveyed restaurant customers in an area similar to those covered by the health department phone surveys. They canvassed 23 fast-food restaurants along Interstate 5 in rural California, asking more than 2,000 customers to identify their zip codes and the towns where they lived. They learned that people who lived within five miles of a restaurant ate out about twice as often as those who lived five to ten miles away, confirming their premise that restaurant visits decreased as the dollar and time costs of traveling for food increased.
The Cost of Consuming
Matsa and Anderson recognized that per-meal costs also influence how much people eat when they visit restaurants. In general, outsized portions are not typically priced significantly higher than more reasonable servings, meaning that cost does not dissuade diners from eating additional calories. In addition, diners are more likely to clean their plates when eating out because their money has already been already spent.
A homemade meal, however, does not prompt the same “I own it, I’m eating it all” response. Those who eat food cooked at home consume less: There is not much to gain by feeding an already-full belly. In economic terms, this is the principle of diminishing marginal utility—the notion that the more you have of something, the less you want still more. If you have just eaten a half-pound of homemade spaghetti, you have probably sated your appetite and are not interested in another serving.
Matsa and Anderson also investigated the role of supply and demand—whether the increase in the number of restaurant meals caused people to consume more calories, or people’s increased caloric demand drove up the number of restaurant meals. They devised a theoretical model to represent consumers’ dining choices, breaking down the factors that influence an eater’s decisions into a simple cost-per-calorie ratio. When their model was altered so both home and restaurant meals were priced equally, some people still ate more than others, reflecting individual preferences. Their results were confirmed by food diaries collected by the U.S. Department of Agriculture, in which people reported what they ate on two nonconsecutive days.
“There is a selection issue,” Matsa explains. “People who eat at restaurants more often might be doing so because they’re hungry for larger meals.” Thus, big eaters eat more no matter where they are, whether at home or dining out.
Although people do eat more when they eat in restaurants, Matsa and Anderson found that diners compensate for those typically highly caloric meals by curtailing what they eat at home during the rest of the day. Again, marginal utility suggests that eating beyond satiety delivers diminishing returns, a result that was empirically supported by the food diaries, according to Matsa. Restaurant meals, while larger, may not have a net effect on calories consumed or body mass. When it comes to obesity, restaurants may not be at fault.
Regulating Repast
While living closer to restaurants increases the frequency of dining out, “restaurants really don’t seem to have a causal effect on body mass,” Matsa says. Without conclusive proof, Matsa and Anderson do not think regulating restaurants is warranted. They calculate that a “sin tax” on restaurant food—like those levied on alcohol and cigarettes and recently proposed for sugary beverages&mmdash;as high as 50 percent would increase the cost of the average restaurant meal by $3.97 but reduce body mass by only 0.004 points. People who eat too many calories will continue to find ways to do so, even when economic pressures limit some of their choices.
“Our work should not be used to trivialize problems related to obesity,” Matsa remarks, “but to promote policies that are more likely to succeed in reducing them.”
Leah Kauffman is a freelance writer based in Pittsburgh, Penn.
Anderson, Michael, and David A. Matsa. 2011. Are restaurants really supersizing America? American Economic Journal: Applied Economics, January, 3(1): 152-188.











