Featured Faculty
William Ocasio was previously a member of the Management & Organizations faculty at Kellogg
The ever-rising cost of health care in the United States has plagued the nation’s economy for years. Elected officials have tried to tackle the problem every so often, and the current health care overhaul making its way through Congress is just the latest attempt. During the debate, legislators cited cost control as one of reform’s more desirable outcomes. And since hospitals receive 31 cents per health care dollar in the United States, reducing hospital costs could make care more affordable. However, the cuts may be more complex than many assume. Creeping costs may be a congenital defect of the U.S. hospital system, according to research by William Ocasio (Professor of Management and Organizations at the Kellogg School of Management).
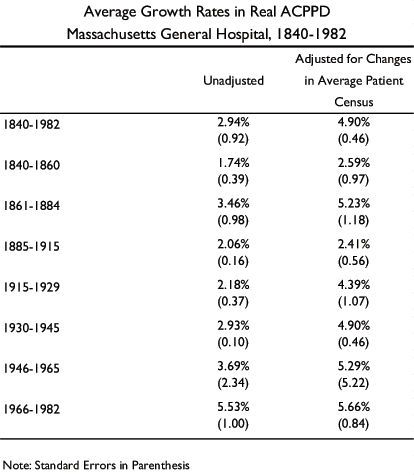
Ocasio analyzed the histories of three hospitals in the Boston area between 1840 and 1980 in his study of American hospitals’ organizational behavior. All three hospitals, like many founded in the eighteenth and nineteenth centuries, began with a focus on philanthropy. But following the Civil War, they and other American hospitals began to shift their attention to medical research in an effort to become leading and respected institutions. Ocasio argues that this drive for institutional greatness has been responsible for the persistent inflation of hospital costs for more than 140 years.
From Humble Beginnings
Many early American hospitals started as philanthropic ventures. Doctors visited middle- and upper-class patients in their homes, and hospitals tended mostly to care for the working poor. Their primary mission was providing charity, not cutting-edge medical care. European hospitals held commanding leads in new medical techniques through most of the nineteenth century, as American hospitals were loath to adopt the latest innovations. For example, Englishman Joseph Lister introduced antiseptic surgical techniques to combat infection in 1867, but Ocasio notes that “antiseptic surgery, which removed germs by carbolic acid spraying, took more than ten years to be introduced in the United States.”
Later in the century, however, American hospitals embraced innovation. Many hospitals that had not adopted antiseptic techniques took up the newer aseptic approach, which attempted to keep harmful bacteria out of surgical chambers in the first place rather than focusing the use of carbolic acid on the instruments and in the wounds. (Though carbolic acid reduced the incidence of gangrene and other infections, it irritated wounds and caused other undesirable side effects.) This advance, in addition to lessons learned caring for the wounded in the Civil War, shifted the paradigm of the American hospital from charity to medical advancement.
Ocasio notes the introduction of aseptic surgery around 1885 was conceptually similar to the adoption of process-flow and assembly-line approaches in manufacturing—both encouraged learning by doing—but their effects on their respective industries differed. “These manufacturing technologies resulted in productivity growth and decreasing costs,” notes Ocasio, but “the ‘experience curve’ of aseptic surgery led to increasing costs.” Aseptic surgeries required substantial investments in both modern facilities and new supplies, including surgical masks, rubber gloves, and sterilization equipment. Other innovations, while improving care, further increased costs. Technologies like X-ray examinations improved diagnostic medicine dramatically, but became yet another expense that decreased hospital revenues.
As the new techniques and procedures improved care, competition increased among elite hospitals. By the end of the nineteenth century, providing charity care had taken a back seat to implementing the latest medical techniques and technologies. The advancement of medicine had become an end in and of itself, Ocasio argues, and procedures were introduced with little to no attention paid to their cost. The few voices that decried outsize hospital spending—advocates of the “efficiency” movement of the early twentieth century—were drowned out.
Searching for a Solution
Still, hospitals were not immune to budgetary concerns. To cope, many hospitals, even those that were founded to serve the poor, increasingly welcomed paying patients. For example, patient payments accounted for only 9 percent of Massachusetts General’s revenue in 1888, but that figure would more than triple by 1905. Even that amount was inadequate, however, as additional paying patients could not stem the losses brought about by expensive technologies.
American hospitals responded not by cutting back on new expenditures, but by increasing the revenue they took in through a variety of ways. For starters, they transformed the way they raised money. “Donations became increasingly defined in terms of their medical efficacy and value rather than as charity donations for the poor,” Ocasio points out. As the twentieth century progressed, American hospitals began to rely more heavily on third-party payors like health insurance plans and government funds, which delayed drastic fiscal action for decades.
Third-party payors became a central part of hospital finances in the mid- twentieth century, but Ocasio believess this dependency enabled rather than caused hospital cost inflation—inflation was intrinsic to a system that valued technological advancement above all else. “The American system of voluntary health insurance emerged as a solution to the [financial] crisis,” Ocasio writes. “Government and third-party payors, rather than becoming an instrument of control over the hospital’s financing and organization, became a source of support for the hospital’s expansion and technological development.”
Early insurance plans helped hospitals cover more costs, but they did not entirely cover their policy holders’ expenditures. It was not until Blue Cross adopted cost-based reimbursement policies that hospitals stopped losing money on insured patients. In 1950 insurance plans paid almost 30 percent of hospital costs. Twenty years later they covered more than 45 percent. Cost-based reimbursement not only saved hospital budgets, it reinforced the role of medical technology in hospital decisions and drove costs even higher.
“The competition for status among hospitals led to competition for technological advancement and the escalation of hospital costs,” Ocasio writes. It led to consistent increases in medical costs throughout his 140-year study. While more recent attempts to bring down costs—like health maintenance organizations (HMOs), hospital systems, and Medicare’s fixed payment system—have provided hospitals with new financing models, he notes, the efficacy of the new approaches “depends on the emergence of a new institutional logic…where hospitals’ status is dependent on efficiency, productivity, and cost control, rather than on new technologies.”
Ocasio, William. 2009. The social construction of hospital-cost inflation. Constructing Markets and Industries. Marc J. Ventresca and Joseph Porac, eds. London: Elsevier Science, Ltd.