Featured Faculty
Professor of Strategy; Herman Smith Research Professor in Hospital and Health Services Management; Director of Healthcare at Kellogg
In 1918 a pandemic flu virus swept across the globe, with disproportionate effects on vulnerable populations, including pregnant women. In the United States 675,000 people were killed by the virus while 25 million contracted it and survived. One in three pregnant women came down with what came to be called the Spanish Flu.
What no one knew at the time were the effects that pandemic flu would have on a mostly-overlooked category of survivors—fetuses in the womb. Since then medical researchers have hypothesized that gestating babies are uniquely susceptible to physical stressors that occur during their development. Nearly a hundred years after the Spanish Flu struck, Craig Garthwaite (Assistant Professor of Management and Strategy at the Kellogg School of Management) used data from the National Health Interview Survey (NHIS) from women who were pregnant during the height of the pandemic in late 1918 and early 1919 to draw new conclusions about the effects of stress on a developing child.
Garthwaite’s analysis could hardly be timelier. Once again, the world is facing a flu pandemic that is especially dangerous to individuals whose immune systems are compromised, including pregnant women. While the H1N1 virus appears to be much less virulent than the strain that struck in 1918, its arrival underlines the outsize impact that the conditions of the first nine months have on the health of individuals for the rest of their lives.
“What you see is a fairly consistent pattern [of long-term health problems] based on the timing of the onset of the flu,” says Garthwaite.
Tell-Tale Trimesters
Garthwaite has discovered that babies whose mothers caught the flu during a particular trimester of their pregnancy were more likely to have health problems affecting the parts of the body that were developing during that trimester.
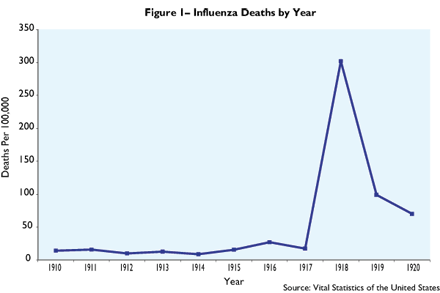
In contrast to earlier research on health outcomes of individuals who were in the womb during prolonged stressors such as famine, Garthwaite’s analysis takes advantage of the intensity and brevity of the 1918 flu pandemic to pinpoint when the flu was most likely to have affected the unborn baby. This allowed Garthwaite to test the hypothesis that the timing of the flu would lead to predictable effects on the unborn child. (See Figure 1 for a graph of flu incidence in the early part of the twentieth century.)
“It’s a fairly strong connection between what the medical literature predicts and the outcome,” says Garthwaite.
The medical literature shows that during the nine months of gestation, the human metabolic system develops early, the heart takes shape slowly in the first and second trimesters, and the kidneys develop in the third. Studies in which rat and other animal mothers are stressed (usually through reduced nutrition) during times that correspond with these developmental phases have shown that the resulting pups have health problems affecting precisely the systems that were developing when the stressor occurred.
Survival Techniques
Researchers hypothesize that the mechanism for these deficiencies work like this: when the fetus is stressed nutritionally, either directly through poor nutrition or indirectly by a disease that saps the mother’s resources, the fetus directs nutrients to the developing brain and away from other organs. From an evolutionary perspective, it makes sense—saving the brain increases the chance the infant will survive until after birth, despite the potential long-term consequences of starving some organs of nutrients during development.
Until Garthwaite’s analysis, no study similar to the animal experiments had been conducted in humans (which would be unethical). By using data from NHIS, which has been conducted continuously since 1957, Garthwaite uncovered statistically significant correlations between individuals’ month of birth, their subsequent health outcomes, and the known peak of the flu pandemic.
In other words, mothers who got the flu early had babies who, decades later, would report problems with diabetes, while mothers who caught the flu in the middle of their pregnancy were more likely to have children who, as adults, would have problems with heart disease. Catching the flu at the tail end of pregnancy increased the odds that a child would grow up to have diseases affecting the kidneys.
The NHIS data does not record the month in which a mother was exposed to the flu, or even whether or not she was, but because the majority of flu cases in the United States happened within such a narrow window of time—a few months—and affected one out of every three pregnant women, Garthwaite was able to uncover a correlation, albeit one that is probably weaker than what he would have found if the actual date of exposure could have been more precisely determined.
A second effect makes it difficult to sort out the actual percentage by which the flu increased incidence of, for instance, heart disease: many of those whose mothers fell ill with the flu during the second half of their pregnancies may not have lived long enough to be included in the survey data Garthwaite used, which start in 1982, when NHIS revised its survey to include more questions.
Prevention Through Public Policy
If future research confirms the results uncovered by Garthwaite—one, by Douglas Almond of Columbia University, already has—then planners who must decide how best to apportion the limited resources of any public health system may take the policy implications of this study seriously.
“The interesting thing for me, as someone who thinks about optimal public program design, is that fetal conditions matter a lot and maybe more than we think they do,” says Garthwaite.
Programs designed to address nutrition at the earliest stages of life, including the Women, Infants, and Children (WIC) program, are underutilized, according to Garthwaite. “We need to be more comprehensive in how we think about the benefits of these programs, because it might help us understand if they’re cost effective and useful,” he says.
Pregnant women in 2009 have much less to worry about than their grandmothers and great grandmothers did in 1918—nutrition is better, medicine has advanced, a vaccine is on the way, and H1N1 appears to be much less harmful than the Spanish Flu ever was—so it is much too early to say whether or not Garthwaite’s work will apply to babies born to mothers exposed to the virus. Among America’s poor and in the developing world, however, UN statistics show that hunger is creeping back up, from an all time low of 800 million to more than a billion. Knowing that the long-term consequences of malnutrition in the smallest portion of a person’s life can determine their health for the rest of it, the tack policymakers take in addressing such issues could have life-long consequences.
Garthwaite, Craig. 2008. The effect of in-utero conditions on long term health: Evidence from the 1918 Spanish Flu pandemic. Working paper